With the expansion of telehealth and similar methods of virtual care, many people, particularly people with disabilities, may have questions about the efficacy and availability of telehealth. A study at the Morehouse School of Medicine’s (MSM) National Center of Primary Care (NCPC) strived to answer these questions.
Led by Megan Douglas, principal investigator and director of research and policy of the NCPC; Mitchell Blount, co-project lead and associate project director of research of the NCPC; and Rasheera Dopson, research assistant, the team received a one-year grant from the Georgia Council on Developmental Disabilities (GCDD) to study the adoption and use of telehealth by people with disabilities in Georgia. The goal was to understand whether and to what extent telehealth has improved access to quality health care services.
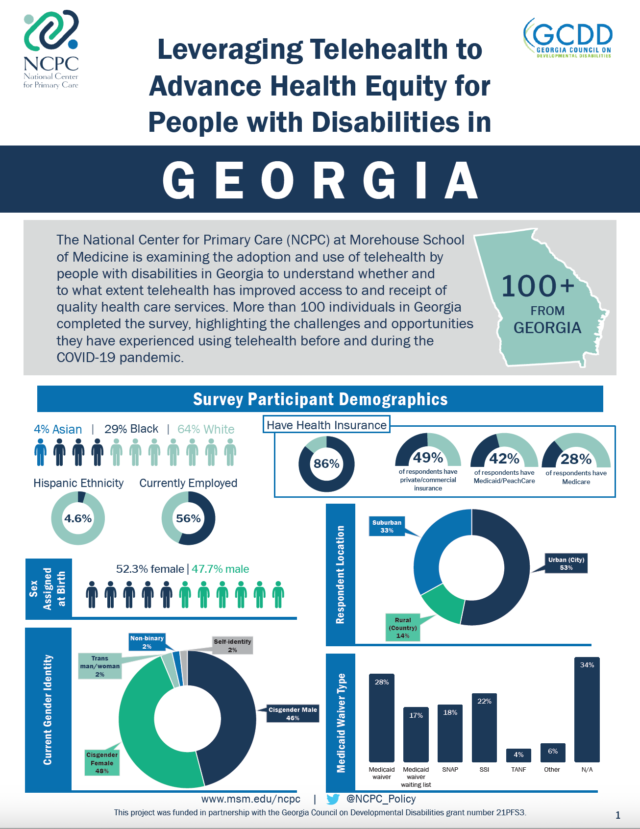
“This study was done in the midst of the COVID-19 pandemic, as we received the grant in 2019. As we know, telehealth was on the rise during this time, but there were not a lot of studies or insights around how people with disabilities were accessing telehealth,” Blount said. “We wanted to make sure that we were helping to assess that impact and make sure that we are able to help support access to care for all people with disabilities in Georgia.”
The team employed a multi-method approach, which consisted of surveys, focus groups, key informant interviews, and a descriptive analysis of policy interventions. According to Blount, the surveys and focus groups focused on people with disabilities, their family members, and direct support professionals.
“We wanted to see how individuals with disabilities were accessing, or not able to access, telehealth and other virtual services, get feedback on what makes a good tool for them, and also gain some provider perspective on barriers and facilitators to actually supporting people with disabilities in accessing care,” said Blount.
 In total, 100 individuals participated in the study’s survey, and 16 individuals participated across six focus groups. The study found that it was difficult to reach people with disabilities who lived in suburban or rural areas due to technological limitations. The group also found that deaf populations often struggled with similar problems.
In total, 100 individuals participated in the study’s survey, and 16 individuals participated across six focus groups. The study found that it was difficult to reach people with disabilities who lived in suburban or rural areas due to technological limitations. The group also found that deaf populations often struggled with similar problems.
“Our study’s deaf population often reported barriers where providers would claim to have the necessary technology available, and when they arrived at their appointments, they did not have it,” Blount said. “About 30% of the study’s deaf population reported encountering such a barrier.”
Another conclusion highlighted by the study was that individuals with physical disabilities are not the only ones who encounter barriers to accessing care. Moreover, the study concluded that the need for equitable telehealth access for people with disabilities is ongoing and must be addressed.
 “Policy and practice changes, including permanent expansion of telehealth and broadband access, access to needed support staff in-and-out of the practice setting, and supports to increase digital literacy and updates in technology, are needed to ensure equitable access to telehealth and virtual services by people with disabilities in Georgia,” Douglas stated.
“Policy and practice changes, including permanent expansion of telehealth and broadband access, access to needed support staff in-and-out of the practice setting, and supports to increase digital literacy and updates in technology, are needed to ensure equitable access to telehealth and virtual services by people with disabilities in Georgia,” Douglas stated.
Although the study has ended, the team at MSM’s NCPC continues to support people with disabilities through their research and initiatives. Their latest endeavor has been to engage and empower people with disabilities to participate in research.
“We have set up an advisory council that is largely composed of people with disabilities,” Blount explained. “Our goal with the council is to assess their needs and potential barriers. We developed this cohort who guided the development of a curriculum to help support people with disabilities and researchers and to serve as a framework for research institutions for future research.”
